Ali Rogin Ali Rogin
Karina Cuevas Karina Cuevas
Leave your feedback
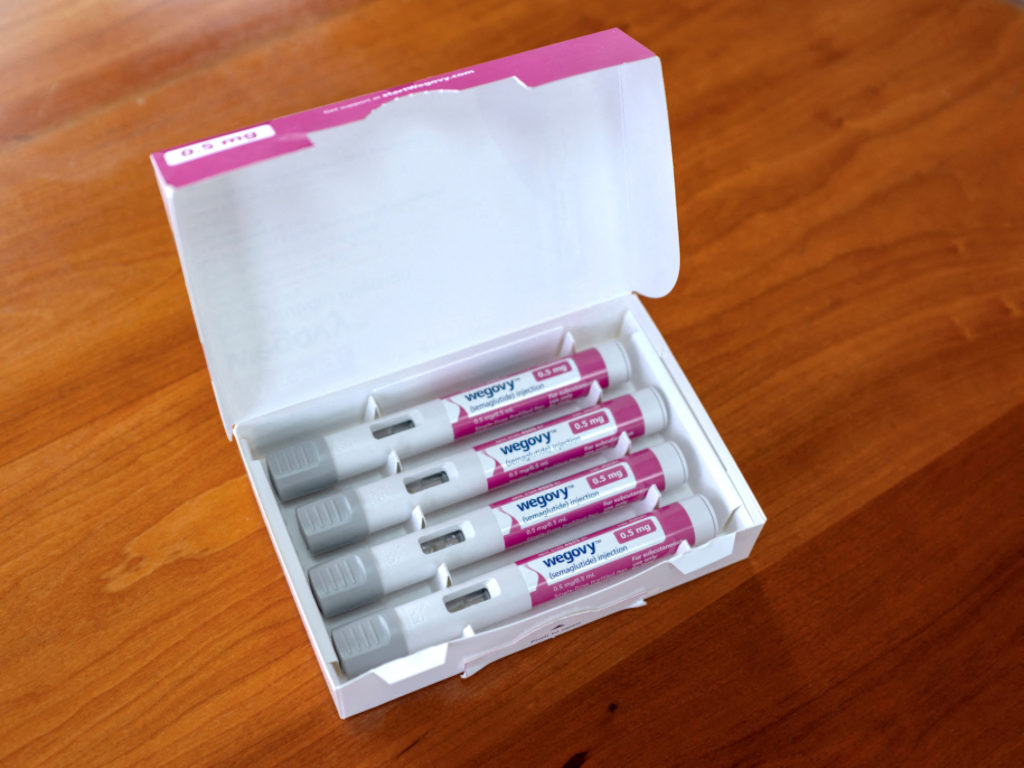
One of the biggest health stories of this past year is the surge in demand for popular weight-loss drugs like Ozempic and Wegovy. Those drugs are in such demand that there’s a nationwide shortage of them. Pharmaceutical companies are scrambling to keep up at a time of rising obesity rates in the U.S. Ali Rogin reports.
Notice: Transcripts are machine and human generated and lightly edited for accuracy. They may contain errors.
Geoff Bennett:
One of the biggest health stories of this past year is the surge in demand for popular weight loss drugs like Ozempic and Wegovy.
In fact, those drugs are in such demand, there’s a nationwide shortage of them. Pharmaceutical companies are scrambling to keep up.
Ali Rogin has a look at the demand and the questions lots of people have about these drugs.
Ali Rogin:
Government surveys show that as much as 40 percent of the U.S. population meets the medical definition of obesity. And, in 22 states, at least 35 percent of adults are obese, mostly in the South and Midwest.
Medications, including the latest FDA-approved drug Zepbound from Lilly, provide hope to patients looking for sustainable weight loss, but they also raise questions related to high costs, insurance coverage and long-term effectiveness. Depending on the drug and insurance, they can cost patients thousands of dollars a year to stay on them. And research suggests people may need to stay on them to maintain that weight loss.
To help look at some of these concerns, I’m joined by Katherine Saunders. She’s an assistant professor of clinical medicine at Weill Cornell Medicine and specialist in obesity and weight-related medical complications at New York Presbyterian Hospital.
Dr. Saunders, thank you so much for joining us.
You prescribe these medications to your own patients. You come up with detailed treatment plans. And I want to talk about all of that. Why have these medications become so popular in recent years? And does it have to do with the medical community’s rethinking of what factors contribute to obesity in some cases?
Dr. Katherine Saunders, Assistant Professor of Clinical Medicine, Weill Cornell Medicine: Yes, so two reasons.
One is that, when I started training over a decade ago, the most effective anti-obesity medications were associated with 5 percent to 10 percent total body weight loss, which is absolutely what we consider to be clinically significant.
If you think about any diet or any behavioral intervention being associated with 3 percent weight loss, on average, 3 to 5, 5 to 10 was pretty good back then. But the medications that have come out over the last few years are considerably more effective, at 15 percent and now upwards of 22 percent.
So, one is the increase in efficacy in the studies and effectiveness that we’re seeing among our patients. And two is that there’s greater recognition that obesity is a disease that requires medical management for the vast majority of people to effectively lose weight and then, more importantly, keep that weight off long term.
Ali Rogin:
And what are some of the risks that are associated with being on these medications?
Dr. Katherine Saunders:
So, each of the medications has its own risk-benefit profile.
Our typical patient has lost and gained weight so many times over the years that they come to us saying: I have been so successful in so many other aspects of my life, and I just absolutely cannot lose weight and keep it off.
So, for somebody like that, who has had a very difficult time losing weight with nonmedical intervention, the risk-benefit profile is really different. So if you take a look at nausea, reflux, constipation, those are the main complications that we’re seeing with GLP-1-type medications. It’s a different risk-benefit profile.
We can absolutely do so much in terms of dietary management, behavioral change to mitigate those side effects. So the hype that we’re seeing is because patients are either on too high a dose, they’re inappropriate candidates. But those side effects generally, if you weigh the risk-benefit profile of having untreated obesity related to so many other health complications, for each person, it’s an individual decision.
Ali Rogin:
You have talked about the importance of coming up with a detailed treatment plan with your patients, looking with them to see if other interventions might work before medication is considered.
Why are those things so important. And are you concerned that right now doctors may be overprescribing these medications?
Dr. Katherine Saunders:
Yes, I think that’s a fabulous question.
There is such a tendency that we’re seeing now to have a health care provider see a patient with obesity and say, oh, I have a medication that can finally help you lose weight. Here’s a prescription for one of the medications without the appropriate education and support and the associated required lifestyle interventions like diet exercise, behavioral change that are really necessary for comprehensive obesity treatment.
So, it’s really not just about one medication to as many people as can be taking this medication. It’s really about seeing each patient as an individual, doing a very thorough evaluation of everything in their history, everything in their medical conditions that are leading to weight gain, everything preventing weight loss, and then optimizing lifestyle.
Ali Rogin:
There’s been a lot of talk about people who want to pursue these drugs to reach a goal weight, and then are planning to get off the drugs and sustain that goal weight with diet and exercise.
What is your take on that approach? Is that sustainable?
Dr. Katherine Saunders:
So, we get so many questions about this. This is a really hot topic right now.
Obesity is a chronic disease, meaning that it doesn’t just go away, meaning that we, unfortunately, right now can’t cure it. Maybe, one day in our lifetime, we will be able to. But if you think about other chronic diseases that you classically think of as chronic diseases, like high blood pressure, high cholesterol, diabetes, people who have these conditions that are not managed by lifestyle intervention alone, expect to start a medication and expect to stay on that medication long term.
So if they stop that medication, their blood pressure goes up, their cholesterol goes up, their blood sugar goes up. And we expect that. With obesity, there’s been this long-held belief that it’s just a lifestyle problem, and that it’s such a massive industry that’s really preying on very vulnerable individuals who are looking for a quick fix or something that can cure their obesity.
We’re not there yet. So, right now, when we start a patient on a medication, it’s a long conversation about the need to take that medication long term. If you take a look at their SURMOUNT-4 trial, which was published in the last few weeks, this trial showed that, when people stopped taking Zepbound, they regained about two-thirds of their body weight over the next several months.
Ali Rogin:
We mentioned that there are shortages of many of these medications.
In your opinion, what needs to change about the availability of these drugs, as well as access to them? Because even for people who can access them, they might not be able to afford them.
Dr. Katherine Saunders:
Yes.
So we have a huge problem right now. It’s not enough that we have FDA approval of these medications. We need better coverage. We need the prices to be lower. And we need more providers who know how to prescribe these medications appropriately.
It’s interesting that Ozempic, which we were using before Wegovy came out in 2021, there really weren’t supply issues until Wegovy hit the market. Wegovy and Ozempic are the same compound, just marketed for weight versus diabetes. And as soon as Wegovy was FDA-approved and people realized that Ozempic was the same medication, we started to see shortages.
So, now that Zepbound is approved — this is the latest one to be approved last month — the medication Mounjaro is the same medication. And so Eli Lilly is concerned about shortages of both of the medications, and they have opened new facilities in order to increase supply, so that we don’t see what we have been seeing with Wegovy and the Ozempic shortages.
But the demand is just so high that it’s a big problem.
Ali Rogin:
A big problem and a very hot topic.
Dr. Katherine Saunders with Weill Cornell Medicine and New York Presbyterian Hospital, thank you so much for your time.
Dr. Katherine Saunders:
Thanks for having me.
Watch the Full Episode
Dec 28
By Amanda Seitz, Associated Press
Nov 08
By JoNel Aleccia, Associated Press
Aug 21
By William Brangham, Karina Cuevas
Aug 13
By JoNel Aleccia, Associated Press
Mar 07
By Michelle Chapman, Associated Press
Ali Rogin Ali Rogin
Ali Rogin is a correspondent with the PBS NewsHour and PBS News Weekend.
Karina Cuevas Karina Cuevas
Support Provided By: Learn more
Subscribe to Here’s the Deal, our politics newsletter for analysis you won’t find anywhere else.
Thank you. Please check your inbox to confirm.
© 1996 – 2024 NewsHour Productions LLC. All Rights Reserved.
Sections
About
Stay Connected
Subscribe to ‘Here’s the Deal,’ our politics newsletter
Thank you. Please check your inbox to confirm.
Learn more about Friends of the NewsHour.
Support for NewsHour Provided By