University of California San Francisco
By Jess Berthold
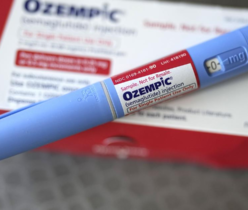
With three-quarters of Americans obese or overweight, interest in weight-loss treatments is at an all-time high. Three injectable medications have dominated the spotlight of late: Wegovy, Ozempic and Mounjaro. These once-a-week, injectable drugs are so popular, in fact, that pharmacies routinely run out of stock.
Many health experts are conflicted about the success of these drugs, however. While life-changing for patients who have long struggled with diabetes, obesity and associated conditions, the medications should not be taken lightly, said Diana Thiara, MD, the medical director of UCSF’s Weight Management program.
Wegovy is FDA-approved for obesity. Ozempic and Mounjaro are FDA-approved for diabetes. However, the manufacturer of Mounjaro is now seeking FDA approval for the drug to be covered for weight management. We hope to hear more about this by the end of the year.
People do lose weight on all three of them, and a lot of physicians are prescribing the diabetes drugs as weight-loss drugs, though that’s not what they are currently approved for.
People on the highest dose of Mounjaro have lost up to 21% of their body weight. For the other two, people lose about 12-15% of body weight.
Past drugs worked mostly in the brain to suppress appetite and help people feel more satisfied with smaller quantities of food. These newer medications work on your brain to make you feel full and also on your body to help keep food in your stomach longer. In addition, they improve your body’s ability to secrete insulin, which controls blood sugar and can help with metabolism.
It’s not dangerous to the individual. These medications have been studied and are safe. But it can be problematic in the sense that prescribing diabetes medications for weight loss contributes to medication supply shortages, so people who need the medications for diabetes can’t always get them. Lower socioeconomic status patients seem to be most affected and already experience more health disparities.
Insurance covers them for their intended use, not for the off-label use. If someone is using Ozempic for weight loss and not diabetes, they are either paying out of pocket or their prescriber wrote “diabetes” as the diagnosis so it could be covered.
They cost around $1,000 a month.
No, these medications for weight loss don’t work that way. There was one study done with Wegovy, called the STEP 4 Trial, that looked at short-term use. Study participants started on the medication for 20 weeks, then, after 20 weeks, half stayed on the medication and half went off. The half who stopped the medication regained almost all of their weight, about 70%, after 48 weeks.
Yes, it seems so. Obesity is a metabolic disease, just like diabetes or hypertension, and it requires long-term attention. In another study of Wegovy, called the STEP 1 extension study, people were given Wegovy for one year. Half the group stopped the medication, and they regained two-thirds of the weight they had initially lost. In the group that stayed on the medication, they kept off all the weight they lost.
First, you need to get prior authorization through insurance – i.e., approval for it to be covered. It’s challenging because insurance companies change what they cover without telling providers or patients when or why or how. Another issue is, if a patient does get Wegovy covered, they must lose 5% of their body weight after five to six months of taking it or else insurance will stop paying for it.
Yes, in California, Medi-Cal covers it. The San Francisco Health Plan covers it. Medicare does not; it is a blanket policy that they don’t cover medications for weight loss. They will cover Ozempic and Mounjaro for diabetes, though.
Supply chain issues have been a consistent problem ever since this drug came to market. We are experiencing supply chain issues right now, again. I tell patients that the first three doses of Wegovy, where you are gradually increasing the amount, are often on backorder. Patients often have to call around to different pharmacies to see what is in stock at that moment, and sometimes the dose is gone by the time the provider fills the order. Sometimes patients can find one or two doses but not the third. I have patients who drive hours from home to get their doses.
Sometimes there is a mild allergic skin reaction at the injection site that can be addressed by a cream or an oral allergy medication. There are also common but not serious side effects, such as nausea, diarrhea, fatigue, constipation and upset stomach. Then there are the rare but serious side effects that affect less than 1% of people. These are things like pancreatitis, cholecystitis, kidney injury and suicidal ideation. It’s because of these that a provider needs to monitor a patient’s symptoms and bloodwork while they are on the medication.
Neither the FDA or pharmaceutical companies have advised on this, but in our weight management clinic we are conservative. We get baseline kidney, liver and lipase function lab tests before starting the medications. We meet with patients every four to six weeks during the first five months when they are increasing their dose to make sure they are not having side effects. Around the second dose, we repeat labs, and then do the labs again at six months, once the patient is at the maximum dose. If everything looks great, we take labs every six months to a year after that.
There are guidelines for prescribing: BMI of at least 30, or at least 27 if there are other health issues. But in practice, whenever you see someone with excess weight, you need to take their whole health picture into account: other illnesses, overall function and whether their health is worsening over time. If someone is on the verge of a medical diagnosis related to weight, it makes sense to treat their obesity pharmaceutically. This is different from the patient who comes in who wants to lose weight but has no health issues or looming health issues, and who might be unhappy with their weight due to social pressure.
Subscribe to UCSF News
Visit the Media Center
© 2024 The Regents of The University of California